Acne does not stop at twenty. If you are still breaking out in your thirties, forties or beyond, this is not unusual, and it is not something to be embarrassed about. Adult acne is one of the most common skin concerns seen by prescribers in the UK, affecting an estimated 54% of women and 40% of men over the age of 25. Unlike teenage acne, which is primarily driven by a surge in androgens during puberty, adult acne is often rooted in a more complex combination of hormonal fluctuations, chronic stress, lifestyle factors, and skin barrier disruption — which is precisely why the spot creams that worked at sixteen are rarely effective at thirty-six. The frustration of dealing with breakouts as an adult is real, valid, and entirely understandable. At The Care Pharmacy, our prescribing team works with adults across the UK every day to find the right clinical approach — because adult acne deserves adult-level treatment.
Before we explore the detail, get in touch with our team if you have questions, or complete our online consultation to find out whether you are eligible for prescription acne treatment.
Start Your Consultation
Quick Answer
Adult acne happens because the same core mechanisms that drive teenage acne — excess sebum, clogged pores, bacterial growth, and inflammation — can persist or re-emerge in adulthood, triggered by hormonal changes, stress, diet, and skincare habits. In adults, hormonal fluctuations linked to the menstrual cycle, pregnancy, perimenopause, polycystic ovary syndrome (PCOS), and changes in contraception are among the most common drivers. Chronic stress elevates cortisol, which in turn stimulates androgen production and sebum output — creating the physiological conditions for breakouts even in adults who had clear skin as teenagers. Adult acne tends to cluster around the lower face, jaw, and chin, which is a hallmark of hormonal involvement. The good news is that effective prescription treatments exist, and adult acne responds well to the right clinical approach.
Why Do Adults Get Acne?
The question of why adults get acne is one that deserves a more honest and thorough answer than most clinical content provides. The standard explanation — “hormones” — is technically accurate but frustratingly incomplete. Adult acne is a multifactorial condition, meaning it rarely has a single cause, and understanding the individual drivers behind your breakouts is the key to finding a treatment that works long-term.
At its core, acne develops through four interconnected processes:
- Excess sebum production: Sebaceous glands produce more oil than normal, often in response to androgenic hormones. This creates the oily skin environment in which acne thrives.
- Follicular hyperkeratinisation: Dead skin cells do not shed from inside the pore as they should, instead accumulating and forming a plug — the foundation of every comedone, papule, and pustule.
- Bacterial proliferation: Cutibacterium acnes colonises the sebum-filled, oxygen-depleted pore and triggers an inflammatory response.
- Inflammation: The immune system responds to bacterial activity within the pore, producing the redness, swelling, and pain that characterises inflammatory acne.
In adults, these processes are set in motion by a different set of triggers than in teenagers. Puberty provides a single, dramatic surge in androgens. Adult acne, by contrast, is driven by subtler, more persistent, and more varied hormonal and lifestyle factors — which is why it is often harder to treat with standard OTC approaches and why it frequently requires clinical intervention to resolve.
Adult Acne Causes: The Full Picture
Understanding adult acne causes means looking beyond the skin surface at what is happening systemically and in your daily life. The following are the most clinically significant contributors to adult breakouts.
Hormonal fluctuations
Hormones are the single most significant driver of adult acne — particularly in women. Androgens (including testosterone and its derivatives) stimulate sebaceous gland activity, and even small fluctuations in androgen levels can trigger excess sebum production and subsequent breakouts. In adults, these fluctuations occur in response to the menstrual cycle, pregnancy, postpartum hormonal changes, perimenopause, and conditions such as PCOS.
Chronic stress and cortisol
The relationship between stress and acne is not anecdotal — it is physiologically well established. Psychological stress activates the hypothalamic-pituitary-adrenal (HPA) axis, triggering the release of cortisol. Cortisol stimulates the adrenal glands to produce androgens, which in turn drive sebum production. Stress also impairs the skin barrier and promotes inflammation, creating the perfect conditions for breakouts. For many adults, stress is the primary driver of their acne — and it is one that is frequently overlooked in treatment planning.
Changes in contraception
Starting, stopping, or switching hormonal contraception is a very common trigger for adult acne. Combined oral contraceptives that contain both oestrogen and a progestogen with low androgenic activity often improve acne by reducing free androgen levels. When these are stopped — or when a patient switches to a progestogen-only pill or a hormonal IUD — the relative increase in androgenic activity can trigger significant breakouts, sometimes for the first time in years.
Diet and blood sugar
The relationship between diet and acne has strengthened considerably in the published evidence over the past decade. High-glycaemic diets — characterised by refined carbohydrates, sugary foods and drinks, and processed snacks — cause rapid spikes in blood glucose, which trigger insulin release and downstream increases in insulin-like growth factor 1 (IGF-1). IGF-1 stimulates sebaceous gland activity and keratinocyte proliferation, both of which contribute directly to acne development. Dairy consumption — particularly skimmed milk — has also been associated with acne in multiple studies, possibly due to the hormonal content of milk or its effects on IGF-1.
Skincare product choices
Comedogenic skincare products — those containing oils, heavy emollients, or occlusive ingredients that block pores — are a surprisingly common cause of adult acne, particularly in patients who are investing heavily in skincare. Rich moisturisers, facial oils, and certain SPF formulations can clog follicles and trigger breakouts in acne-prone adults, even when the products themselves are marketed as suitable for sensitive or mature skin.
Sleep deprivation
Insufficient or poor-quality sleep increases systemic inflammation, elevates cortisol levels, and impairs the skin’s overnight repair processes. Adults who are chronically sleep-deprived are more likely to experience persistent breakouts that do not respond well to topical treatment, because the underlying inflammatory state is being perpetuated from within.
Hormonal Acne in Adults: What Is Really Going On?
Hormonal acne in adults has a characteristic pattern that distinguishes it from other types of adult acne, and recognising that pattern is clinically important because it points towards the most effective treatment approach.
The hallmarks of hormonal adult acne include:
- Distribution: Predominantly along the lower face — the jawline, chin, and neck. This is the area most responsive to androgenic stimulation of the sebaceous glands and is the most reliable indicator of hormonal involvement.
- Cyclical timing: Many women notice a clear relationship between their breakouts and their menstrual cycle, with flares typically occurring in the week before menstruation when progesterone peaks and oestrogen falls, creating a relative androgenic dominance.
- Type of lesion: Hormonal acne often produces deep, tender, cystic nodules rather than surface-level pustules. These sit beneath the skin surface, are slow to resolve, and are more likely to leave post-inflammatory hyperpigmentation.
- Persistence: Hormonal acne tends to be chronic and resistant to OTC treatments, because topical products cannot address the systemic hormonal drivers.
Hormonal acne and PCOS
Polycystic ovary syndrome (PCOS) is one of the most commonly underlying conditions in women presenting with persistent adult acne. PCOS is characterised by elevated androgen levels, which drive sebaceous gland activity and produce the classic pattern of deep jawline and chin acne. Acne that is severe, persistent, and accompanied by other features such as irregular periods, excess facial or body hair, or weight gain warrants investigation for PCOS via a GP referral, blood tests, and ultrasound.
Perimenopause and acne
The perimenopause — the transitional period leading up to the menopause, typically beginning in the mid-to-late forties — is an increasingly recognised trigger for adult acne. As oestrogen levels decline, the relative androgenic effect on the skin increases, driving a resurgence of acne in women who may have had clear skin for decades. Perimenopausal acne is frequently misunderstood and undertreated, partly because patients and clinicians may not immediately connect the two. If you are experiencing new or worsening acne alongside other perimenopausal symptoms, get in touch with our team to discuss your options.
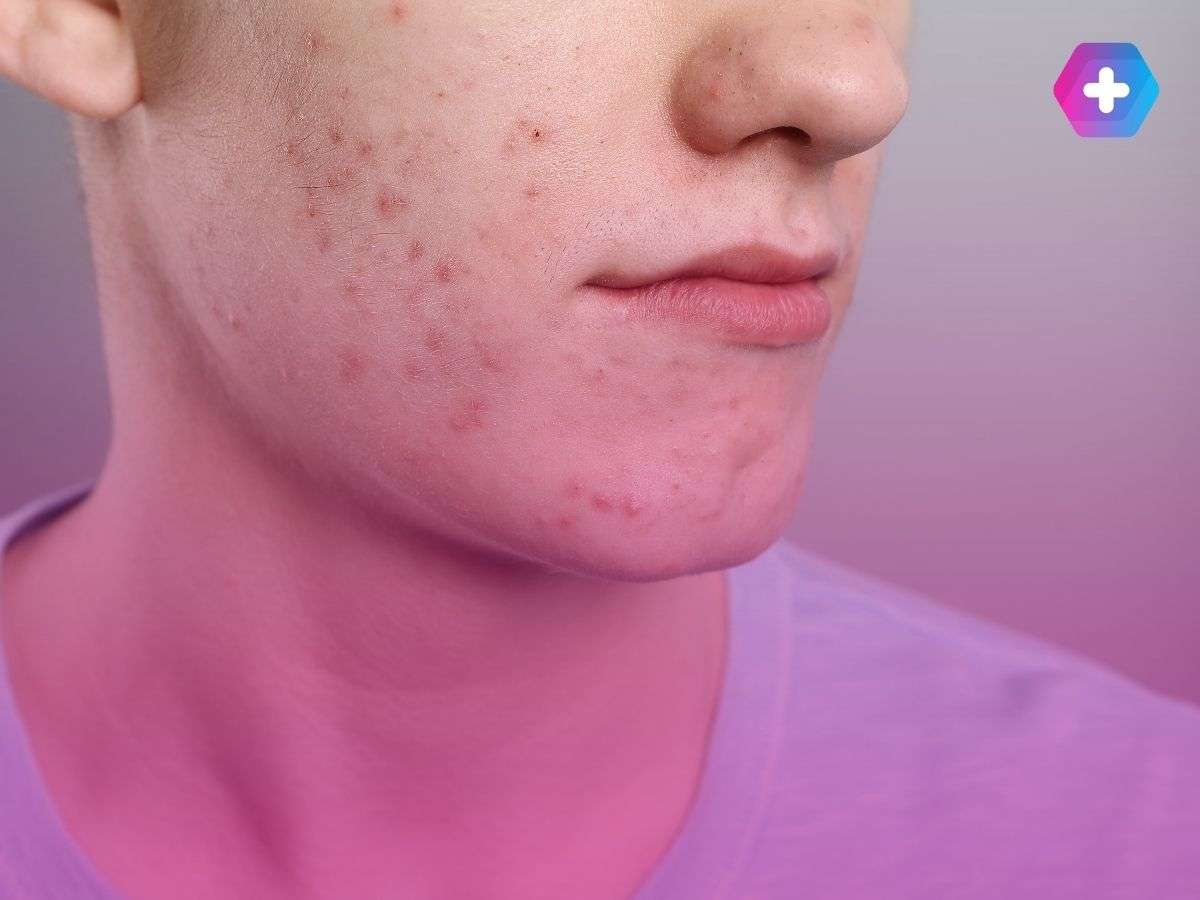
Why Am I Getting Acne in My 30s?
If you are asking why am I getting acne in my 30s, you are in very good company. Research consistently shows that acne in the thirties is not a rarity — it is one of the most common skin concerns presenting to dermatologists and online prescribing services in the UK. The thirties represent a unique hormonal and lifestyle context that creates ideal conditions for adult acne to develop or persist.
Several factors converge in the thirties to make this decade particularly acne-prone:
- Peak stress years: Career pressure, financial demands, and for many, the physical and psychological demands of pregnancy or early parenthood create a cortisol environment that persistently elevates androgen production and inflammation.
- Contraception changes: Many women stop hormonal contraception in their thirties to conceive, or switch methods — and the hormonal transition that follows can trigger significant breakouts that persist for months.
- Postpartum hormonal shifts: The dramatic hormonal changes following childbirth — particularly the drop in oestrogen and progesterone — frequently trigger postpartum acne that can last for many months, especially in breastfeeding women.
- Skincare overload: The thirties are also the decade when many people begin investing seriously in skincare — retinoids, acids, vitamin C serums, rich moisturisers — and the introduction of multiple new actives can trigger purging, sensitisation, or comedone formation.
- Declining cell turnover: From the late twenties onwards, the rate at which skin cells turn over begins to slow, meaning dead cells are more likely to accumulate within the follicle and contribute to comedone formation.
The important message is this: acne in your thirties is not a sign of poor hygiene, bad skincare choices, or something fundamentally wrong with your health. It is a physiological response to a specific set of triggers — and with the right clinical approach, it is entirely treatable. Complete our online consultation to find out which treatment is right for you.
Adult Acne vs Teenage Acne: Key Differences
The reason so many adult acne sufferers find that standard spot treatments fail them comes down to one thing: adult acne is a fundamentally different condition to teenage acne and needs to be treated accordingly.
Feature
Teenage Acne
Adult Acne
Primary driver
Pubertal androgen surge
Hormonal fluctuations, stress, lifestyle, diet
Distribution
Forehead, nose, chin (T-zone)
Jawline, chin, neck, lower cheeks
Skin type alongside acne
Usually oily throughout
Often combination or dry skin with breakouts
Lesion type
Surface pustules and blackheads common
Deep, cystic nodules more common
Natural resolution
Often improves after puberty
Unlikely to resolve without treatment
Response to OTC products
Often adequate for mild cases
Frequently insufficient — prescription treatment often needed
Skin sensitivity
Generally more resilient
Often more reactive — harsh treatments cause irritation
Scarring risk
Moderate
Higher — adult skin heals more slowly and scars more readily
Emotional impact
Significant
Often more distressing due to social and professional context
Adult Acne Treatment: What Actually Works
The most important shift in thinking about adult acne treatment is this: adult acne is not a less serious version of teenage acne. It is a distinct clinical presentation that requires a treatment plan matched to its specific drivers. The following framework reflects how our prescribing team approaches adult acne in clinical practice.
Step 1: Address the trigger
Before reaching for a product, consider what might be driving your breakouts. If you have recently changed contraception, are under significant stress, or have introduced a new skincare product, these are the most likely culprits and addressing them directly will yield better results than any topical treatment alone. A symptom diary — noting when breakouts occur, their location, and any correlating life events or product changes — is an invaluable tool.
Step 2: Simplify and rebuild your skincare routine
One of the most common mistakes adult acne sufferers make is overloading their skin with too many active ingredients at once. A foundational routine for adult acne-prone skin should include:
- A gentle, non-comedogenic, fragrance-free cleanser used twice daily
- A lightweight, oil-free, non-comedogenic moisturiser applied morning and evening
- A broad-spectrum, non-comedogenic SPF 30 or higher applied every morning
- A targeted active ingredient — either retinoid or a combination prescription product — applied as directed
Step 3: Consider over-the-counter actives
For mild adult acne, OTC ingredients including benzoyl peroxide (2.5–5%) and salicylic acid (0.5–2%) can be effective starting points. However, adult skin is often more sensitive than teenage skin, meaning lower concentrations and less frequent application are advisable when starting out. If OTC products have not produced meaningful improvement within eight to twelve weeks, prescription treatment is the appropriate next step.
Step 4: Seek prescription treatment
For the majority of adult acne patients — particularly those with moderate-to-severe acne, jawline-predominant hormonal acne, or deep cystic lesions — prescription treatment is not simply an upgrade. It is the clinically appropriate standard of care, and it is available through a simple online consultation with our prescribing team.
Prescription Treatments for Adult Acne
The following prescription treatments are available following a confidential online consultation and represent the most clinically effective options for adult acne in the UK.
Epiduo (adapalene 0.1% + benzoyl peroxide 2.5%)
Epiduo is a fixed-dose combination gel that addresses two of the core mechanisms of adult acne simultaneously. Adapalene — a third-generation retinoid — normalises skin cell turnover within the follicle, preventing the dead cell accumulation that leads to blocked pores. Benzoyl peroxide kills C. acnes directly and prevents the antibiotic resistance that can develop with antibiotic monotherapy. Applied once daily in the evening, Epiduo is particularly well suited to adult patients with mixed acne — both comedonal and inflammatory — and those who have not responded adequately to OTC products.
If your skin is on the sensitive side, starting with every other evening application and gradually increasing to nightly use can significantly reduce the initial irritation that often occurs in the first few weeks of treatment.
Duac (clindamycin 1% + benzoyl peroxide 5%)
Duac is a once-daily combination gel that pairs the topical antibiotic clindamycin with benzoyl peroxide. This combination is particularly effective for inflammatory adult acne characterised by red papules and pustules — the type of breakout most commonly seen in jawline and chin acne with a hormonal driver. The inclusion of benzoyl peroxide alongside the antibiotic is clinically important, as it significantly reduces the risk of C. acnes developing resistance to clindamycin over time.
Duac is generally well tolerated by adult skin. Some initial dryness and mild peeling is common in the first two weeks and usually settles as the skin adapts.
Lymecycline (oral antibiotic)
Lymecycline is an oral tetracycline antibiotic that is highly effective for moderate-to-severe inflammatory adult acne, or for acne that is too widespread or deep-seated for topical treatment alone to address. It is typically prescribed for a minimum of twelve weeks and often continued for up to six months, usually alongside a topical treatment such as Epiduo to maximise results and minimise the risk of resistance development.
For adult patients with hormonal acne — particularly deep, cystic jawline breakouts — lymecycline combined with a topical retinoid is often the most effective non-hormonal prescription approach. It is generally well tolerated, though patients should take it with a full glass of water and maintain an upright position for at least 30 minutes after taking it.
All three treatments are available following a confidential online consultation with our prescribing team.
Ten Practical Steps to Help You Manage Adult Acne More Effectively
Getting on top of adult acne is about combining the right clinical treatment with the right daily habits. Here are ten evidence-informed strategies specifically relevant to adult acne:
- Accept that adult acne requires adult-level treatment. If you have been using products designed for teenage skin — high-strength benzoyl peroxide wash-off products, harsh toners, or mattifying spot treatments — it is time to reassess. Adult skin needs a gentler, more targeted approach that preserves the skin barrier while treating active breakouts.
- Track your breakouts in relation to your cycle. If you menstruate, keep a note of where breakouts appear and when in your cycle they occur. A consistent pattern of jawline and chin breakouts in the week before your period is strong evidence of hormonal involvement and will help guide clinical decisions about treatment.
- Reduce high-glycaemic foods as a genuine clinical intervention. Swapping refined carbohydrates, sugary drinks, and processed foods for lower-GI alternatives — wholegrains, legumes, vegetables — has real evidence behind it for reducing acne severity. This is not about perfection; even modest dietary changes can produce measurable skin improvement over eight to twelve weeks.
- Address stress actively, not aspirationally. If stress is a clear driver of your breakouts, managing it must be part of your treatment plan. Regular physical exercise, consistent sleep, and evidence-based stress management techniques such as CBT or mindfulness have all been shown to reduce cortisol-driven skin inflammation.
- Audit your skincare for comedogenic ingredients. Check your moisturiser, SPF, foundation, and any facial oils for ingredients including coconut oil, isopropyl myristate, algae extracts, and heavy silicones — all of which can block pores in acne-prone adults. Non-comedogenic labelling is a useful guide but not a guarantee.
- Never skip SPF. Adults using prescription acne treatments — particularly retinoids — are significantly more photosensitive. Daily broad-spectrum SPF use is non-negotiable, both to protect the skin during treatment and to prevent post-inflammatory hyperpigmentation from darkening following breakouts.
- Be consistent and patient with prescription treatments. Adult acne treatments require a minimum of twelve weeks of consistent daily use before meaningful improvement is visible. Stopping and restarting, or switching products every few weeks because you do not yet see results, is one of the most common reasons treatment fails.
- Investigate whether your contraception is contributing. If your acne worsened after stopping or switching hormonal contraception, this is clinically relevant information. Discuss with your GP or prescriber whether your current contraceptive method is the most appropriate choice given your skin concerns.
- Treat post-acne marks as a separate but manageable concern. The dark marks and red spots left after adult acne resolves — post-inflammatory hyperpigmentation — are not scars, and they do respond to treatment. A retinoid applied consistently over several months is one of the most effective approaches, alongside daily SPF use to prevent further darkening.
- Do not let embarrassment delay treatment. Adult acne has a well-documented impact on mental health, self-esteem, and quality of life — and those effects are just as real and valid as the physical symptoms. If your acne is affecting your confidence, your social life, or your willingness to engage professionally, that is reason enough to seek clinical support promptly. Complete our online consultation and let our team help.

Frequently Asked Questions
We hear the same questions about adult acne time and again. Here are the most common ones, answered directly and in plain English:
Is it normal to still have acne in your 30s and 40s?
Yes — completely normal and extremely common. Studies consistently show that acne affects a significant proportion of adults well into their thirties, forties, and beyond, with women more commonly affected than men in adulthood due to cyclical hormonal fluctuations. Adult acne is not a sign of poor hygiene, bad diet, or anything fundamentally wrong with your health — it is a physiological response to a specific set of internal and external triggers that are entirely manageable with the right treatment.
Can hormonal acne in adults be treated without going on the pill?
Yes — for patients who do not want to use hormonal contraception, prescription topical treatments and oral antibiotics such as lymecycline can produce significant improvement in hormonal acne, particularly when combined with lifestyle modifications addressing stress, diet, and sleep. For women with severe hormonal acne or suspected PCOS, a GP referral for hormonal investigation may be appropriate, as there are additional treatment options available within that context.
Why is my adult acne worse around my jaw and chin?
Jawline and chin acne in adults is the classic presentation of hormonally driven acne, as these areas contain a high concentration of sebaceous glands that are particularly sensitive to androgenic stimulation. The lower face is also in close proximity to the neck lymph nodes and is influenced by androgen levels in a way that the forehead and T-zone are not, which is why hormonal fluctuations — including those linked to the menstrual cycle, PCOS, or perimenopause — reliably produce breakouts in this area.
How long does adult acne treatment take to work?
Most prescription acne treatments require a minimum of eight to twelve weeks of consistent daily use before meaningful clinical improvement is visible, with full results typically seen at the twelve to sixteen week mark. Adult patients sometimes see slower initial progress than teenagers due to differences in skin cell turnover rate, but results with prescription treatment are typically sustained and clinically significant when treatment is maintained consistently.
Can stopping the contraceptive pill cause adult acne?
Yes — this is one of the most commonly reported triggers for adult acne, particularly in women who were on a combined oral contraceptive that suppressed androgen activity. When the pill is stopped, androgen levels rebound and sebaceous gland activity increases, often producing significant breakouts that can persist for three to twelve months while the body’s hormonal balance re-establishes itself. Prescription treatment during this transition period can significantly reduce the severity and duration of post-pill acne.
Does diet really affect adult acne?
The evidence linking diet and acne has strengthened considerably in recent years, with high-glycaemic diets and dairy consumption — particularly skimmed milk — most consistently associated with increased acne severity. While dietary changes alone are unlikely to resolve moderate-to-severe acne, reducing high-GI foods and dairy intake alongside appropriate clinical treatment is a well-supported adjunct strategy that can produce meaningful improvement in overall skin condition.
You Deserve Skin That Works for You
Every effective adult acne treatment plan begins in the same place: understanding what is actually driving your breakouts and matching that with a treatment approach built for adult skin. Adult acne is not a teenage problem you have failed to grow out of — it is a distinct clinical condition with specific drivers, a characteristic presentation, and highly effective treatments available when the right clinical approach is taken.
Our pharmacist-led prescribing team is here to help you find the right approach for your skin, quickly and confidentially. Whether you are dealing with cyclical hormonal breakouts, stress-driven flares, or persistent acne that has simply never responded to anything you have tried, we are here to help you find a treatment that actually works — quickly, confidentially, and entirely online.
Reach out to our team today, or complete our online consultation to explore which prescription acne treatments are right for you.
Epiduo (adapalene + benzoyl peroxide)
A dual-action prescription gel combining a third-generation retinoid with benzoyl peroxide for simultaneous comedonal and inflammatory acne treatment. Clinically proven to outperform either ingredient used alone. Applied once daily in the evening. Suitable for adult acne including mixed and persistent presentations.
Available following an online consultation at The Care Pharmacy — view our prescription acne range.
Duac (clindamycin + benzoyl peroxide)
A once-daily combination gel effective for inflammatory adult acne including jawline and chin breakouts. Pairs an antibiotic with benzoyl peroxide to maximise efficacy and reduce antibiotic resistance risk. Well tolerated by adult skin.
Available following an online consultation at The Care Pharmacy.
Lymecycline (oral antibiotic)
An oral tetracycline antibiotic for moderate-to-severe inflammatory adult acne or cases where topical treatment alone is insufficient. Prescribed for a minimum of twelve weeks, usually alongside a topical treatment for optimal results.
Available following an online consultation at The Care Pharmacy.
Stop letting adult acne call the shots
Begin a free, confidential online consultation with our pharmacist-led team. Prescription treatments for adult acne including Epiduo, Duac, and Lymecycline available following assessment.
This article was written by Pharmacy Mentor and clinically reviewed by Mohammed Ismail Lakhi, MPharm, MRPharm, Superintendent Pharmacist at The Care Pharmacy. Mohammed is registered with the General Pharmaceutical Council (GPhC registration number 2072815) and leads clinical governance across The Care Pharmacy’s weight management services.
Last reviewed: May 2026
Disclaimer: This article is for general information only and is not a substitute for individual medical advice. Always consult a qualified prescriber before starting any prescription weight loss treatment.
Medically reviewed by
Mohammed Lakhi
Superintendent Pharmacist








