If you are trying to understand whether you have contact dermatitis vs eczema — or whether your skin condition is an allergic reaction or something else — you are not alone. These two conditions are frequently confused because they can look almost identical, yet they have different triggers, causes, and treatment approaches. The short answer is this: eczema (also called atopic dermatitis) is a chronic condition often linked to genetics and immune sensitivity, while contact dermatitis is caused by direct contact with an irritant or allergen. Knowing the difference matters because the right diagnosis leads to the right treatment. At The Care Pharmacy, our prescribing team supports patients across the UK with clinically appropriate treatments for both conditions — and we are here to help you take the next step.
Before we dive into the detail, get in touch with our team if you have questions about your skin, or complete our online consultation to find out which treatments may be right for you.
Start Your Consultation
Quick Answer
Contact dermatitis and eczema are both inflammatory skin conditions that cause redness, itching, and irritation — but they are not the same thing. Eczema (atopic dermatitis) is a chronic condition driven by a dysfunctional skin barrier and immune response, often running in families alongside asthma and hay fever. Contact dermatitis, by contrast, is a reaction triggered by direct contact with a specific substance — either an irritant or an allergen. While eczema tends to appear in characteristic locations such as the inner elbows and behind the knees, contact dermatitis typically appears where skin has been exposed to the offending substance. Both conditions are treatable with the right clinical approach.
What Is Eczema?
Eczema — most commonly referred to as atopic dermatitis — is a long-term skin condition that causes the skin to become dry, itchy, cracked, and inflamed. It affects around 1 in 5 children and 1 in 10 adults in the UK, making it one of the most prevalent skin conditions in the country.
The underlying cause of eczema is a combination of genetic and environmental factors. People with eczema tend to have a weakened skin barrier, which allows moisture to escape and irritants and allergens to enter more easily. This disruption triggers an immune response, leading to the characteristic inflammation and itch.
Key characteristics of eczema include:
- Chronic and recurring — it flares and settles over time rather than appearing once in response to a specific trigger
- Often associated with the “atopic triad” — asthma, hay fever (allergic rhinitis), and eczema frequently occur together in the same individual or family
- Typically affects the inner elbows, backs of knees, neck, wrists, and face — though it can appear anywhere
- Skin is often dry and sensitive even between flares
- Usually first appears in childhood, though adult-onset eczema is also possible
- Symptoms tend to worsen in cold or dry weather, with stress, or after exposure to certain fabrics, soaps, or skincare products
It is important to understand that eczema is not an allergy in the traditional sense — although people with eczema are more prone to developing allergic sensitivities over time. Eczema is better understood as a skin barrier dysfunction combined with an overactive immune system.
Contact Dermatitis vs Eczema: Key Differences
The table below summarises the most clinically significant differences between contact dermatitis and eczema:
Feature
Eczema (Atopic Dermatitis)
Contact Dermatitis
Cause
Genetic skin barrier dysfunction and immune dysregulation
Direct contact with an irritant or allergen
Duration
Chronic, lifelong condition with flares and remissions
Often resolves when trigger is identified and removed
Location
Inner elbows, knees, neck, wrists — often symmetrical
Wherever skin has touched the offending substance
Onset
Often begins in childhood
Can occur at any age, even after years of safe exposure
Family history
Common — often linked to asthma and hay fever
Not typically relevant
Diagnosis
Clinical — based on history, appearance, and pattern
Patch testing can confirm allergic type
Skin between flares
Often dry and sensitive
Usually normal once trigger is removed
Treatment goal
Ongoing management and flare prevention
Identify and eliminate the trigger; treat symptoms
Is It Eczema or Dermatitis? How to Tell
One of the most searched questions in UK skincare is is it eczema or dermatitis — and with good reason. The two can appear remarkably similar on the surface, with both causing red, inflamed, itchy skin that may weep, crust, or become thickened over time.
Here are some practical questions to help distinguish between them:
- Did your symptoms appear suddenly in one specific area? If so, contact dermatitis is more likely — especially if you recently started using a new product, wore a new piece of jewellery, or began a new job involving chemical exposure.
- Do you have a personal or family history of asthma or hay fever? This significantly increases the likelihood of eczema, as the three conditions frequently co-exist.
- Is the rash in a typical eczema location — inside the elbow, behind the knees, on the neck or wrists — or is it in an unusual pattern that follows a point of contact (such as a watch strap, waistband, or where a cream was applied)?
- Does the rash clear completely between episodes, or does the skin remain dry and sensitive even when not actively flaring? Eczema skin is rarely entirely normal, whereas contact dermatitis typically resolves once the trigger is removed.
- Have you recently introduced anything new into your routine? A new moisturiser, laundry detergent, rubber gloves, or even a new brand of wipes could be responsible if you are experiencing contact dermatitis.
If you are unsure, a clinical assessment — including a detailed history and, if relevant, a patch test — is the most reliable way to differentiate between the two. Our prescribing team can review your symptoms and guide you towards the most appropriate next steps. Get in touch if you would like to discuss your symptoms.
Eczema vs Allergic Reaction: What Is the Difference?
The question of eczema vs allergic reaction is also common — and slightly more nuanced than it might initially appear.
Eczema is not a classic allergic reaction, though it shares some immune system involvement. In a typical allergic reaction (such as hives triggered by a food or drug), the immune system releases histamine rapidly in response to a perceived threat. In eczema, the immune response is more complex and chronic — it involves a dysregulated immune pathway (particularly a type 2 inflammatory response mediated by cytokines such as IL-4 and IL-13) rather than a straightforward histamine release.
Key distinctions:
- Allergic reactions (such as hives, also known as urticaria) typically appear quickly — within minutes to hours — and usually resolve within 24–48 hours without treatment. They are often accompanied by other symptoms such as swelling, sneezing, or a runny nose.
- Eczema flares develop more slowly — often over hours or days — and do not resolve quickly without appropriate management. The skin remains compromised even after visible redness settles.
- Allergic contact dermatitis sits somewhere in between — it is a true allergic reaction (a type IV delayed hypersensitivity reaction), but unlike immediate allergic responses, it takes 24–72 hours to appear after exposure to the allergen.
People with eczema are statistically more likely to develop allergic sensitivities over time due to their impaired skin barrier, which allows allergens to enter more easily. This means that for some patients, eczema and allergic contact dermatitis can co-exist — making accurate diagnosis particularly important.
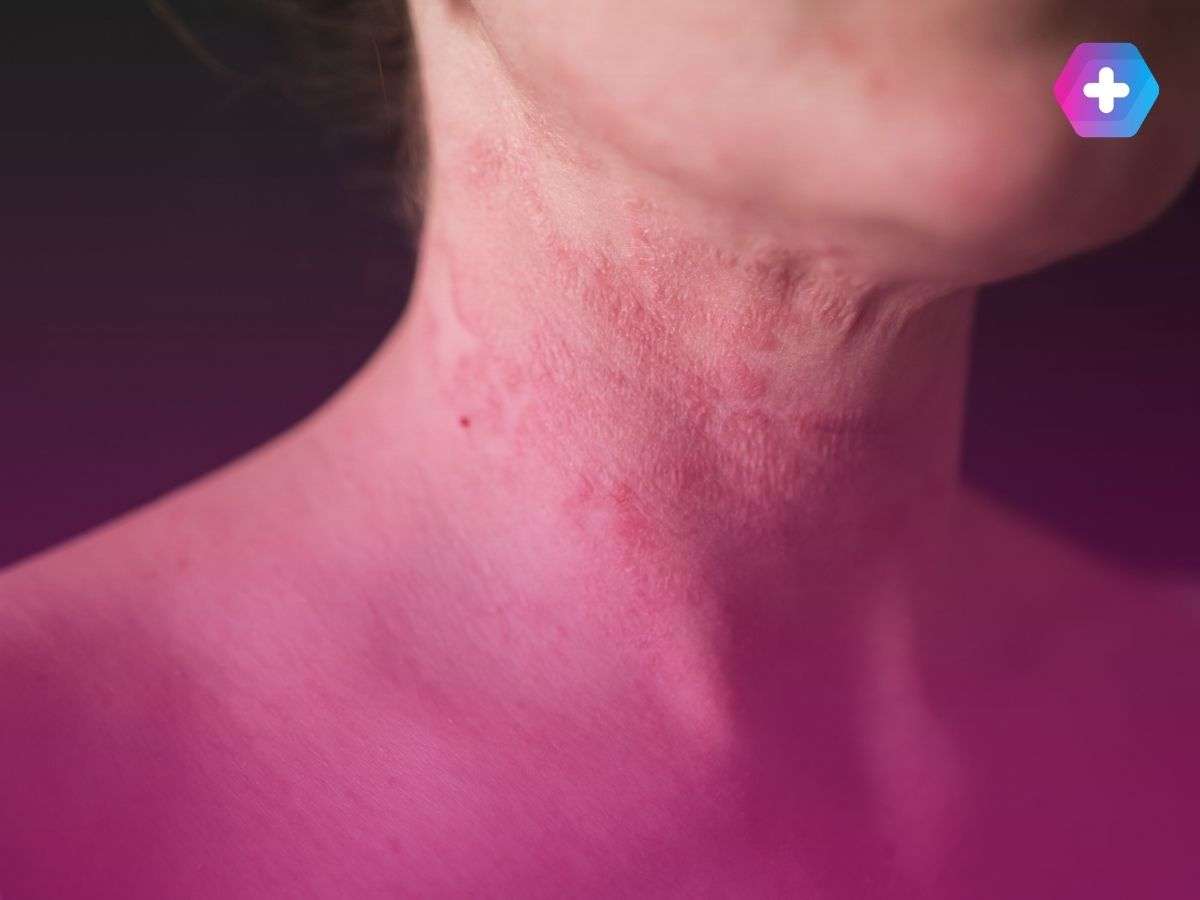
Common Triggers for Each Condition
Understanding what triggers your skin condition is central to managing it effectively. Below are the most commonly reported triggers for each:
Eczema triggers:
- Soaps, bubble baths, and shampoos with harsh detergents or fragrances
- Synthetic fabrics, particularly polyester and nylon; wool can also irritate sensitive skin
- Extreme temperatures — very hot or cold weather, and overheating during exercise
- Stress and anxiety, which can trigger or worsen flares through immune pathway disruption
- Dry air, particularly during winter or in centrally heated environments
- Certain foods (more common in young children with eczema) — including dairy, eggs, and nuts
- Dust mites, pet dander, pollen, and mould
Contact dermatitis triggers:
- Nickel — one of the most common allergens, found in jewellery, belt buckles, watch clasps, and clothing fastenings
- Fragrances in perfumes, cosmetics, and skincare products
- Preservatives in creams and lotions — particularly methylisothiazolinone (MI) and parabens
- Hair dye chemicals — particularly para-phenylenediamine (PPD)
- Rubber latex — occupational exposure in healthcare workers is a significant cause
- Cleaning products, solvents, and detergents — prolonged or repeated skin contact is a key risk factor
- Topical antibiotics and antiseptics — neomycin and lanolin are known sensitisers
Treatment Options for Eczema and Dermatitis
There is no one-size-fits-all approach to treating eczema or dermatitis — the right treatment depends on the type, severity, and location of your condition. However, there are several well-established options that form the foundation of management for both conditions.
Emollients (moisturisers)
Emollients are the cornerstone of both eczema and contact dermatitis management. They help restore and maintain the skin barrier, reduce moisture loss, and prevent the dryness that can trigger flares. They should be applied liberally and frequently — including immediately after bathing while the skin is still slightly damp.
Topical corticosteroids
Topical steroids are the most commonly prescribed treatment for both eczema flares and inflamed contact dermatitis. They work by reducing inflammation in the skin and are available in different strengths — from mild (such as hydrocortisone 1%) to potent (such as betamethasone). The correct strength depends on the affected body area and severity of symptoms.
Betnovate (betamethasone valerate 0.1%) is a potent topical corticosteroid available following a clinical consultation at our pharmacy. It is appropriate for short-term use on moderate-to-severe flares affecting the body — but should not be used on the face or thin skin areas without specific clinical guidance.
Eumovate (clobetasone butyrate 0.05%) is a mild-to-moderate topical steroid suitable for more sensitive skin areas, including the face (with appropriate guidance). It offers effective anti-inflammatory relief with a lower risk profile than stronger steroids.
Antihistamines
Oral antihistamines do not treat the underlying inflammation of eczema or contact dermatitis, but they can provide meaningful relief from itch — particularly at night. Sedating antihistamines (such as chlorphenamine) may be useful for patients whose sleep is severely disrupted by itching.
Barrier repair and specialist creams
Products specifically designed to repair the skin barrier — including those containing ceramides, niacinamide, and colloidal oatmeal — can be helpful for ongoing maintenance between flares. These are particularly useful for patients who experience frequent or prolonged episodes of contact dermatitis due to occupational exposure.
If your symptoms are not responding to over-the-counter options, or if you are unsure which treatment is right for your skin, complete our online consultation to speak with our prescribing team.
Hints and Tips for Managing Eczema and Contact Dermatitis
Managing either condition is not just about medication — everyday habits play a crucial role in reducing flares and protecting your skin barrier. Here are ten evidence-informed tips to help:
- Apply emollients at least twice daily, even when your skin appears clear. Consistent moisturisation is the single most effective way to prevent flares in both conditions.
- Switch to fragrance-free, soap-free cleansers for washing hands, bathing, and showering. Many standard soaps contain detergents that strip the skin’s natural oils and worsen both conditions.
- Wear cotton next to the skin wherever possible. Synthetic fabrics and wool can cause friction and irritation that worsens eczema in particular.
- Keep a symptom diary to identify your triggers. Note when flares occur, what products you have used, what you have eaten, and what you have come into contact with — this information is invaluable when consulting a clinician.
- Use lukewarm water for bathing, not hot. Hot water removes natural oils and can trigger or worsen inflammation. Keep baths and showers brief — ideally no longer than 10 minutes.
- Rinse clothing thoroughly after washing. Residual detergent in fabric is a common but overlooked trigger for both eczema and contact dermatitis.
- Apply topical steroids correctly. Use the fingertip unit guide: one fingertip unit (the amount squeezed from the tip of the index finger to the first crease) covers an area approximately twice the size of your palm.
- Manage stress actively. Stress is a well-documented trigger for eczema flares. Mindfulness, regular exercise, and adequate sleep all contribute to better skin outcomes.
- Protect your hands at work if you are in an occupation that involves frequent hand washing or chemical exposure. Use barrier creams before and after exposure, and apply emollient at the end of each shift.
- Seek a clinical review if your symptoms are not improving. Uncontrolled eczema or dermatitis can lead to secondary infections, significant quality-of-life impact, and progressive skin damage. Our team is here to help — get in touch at any time.
Frequently Asked Questions
Got questions about contact dermatitis and eczema? Here are the answers our patients ask us most often:
Can you have eczema and contact dermatitis at the same time?
Yes — it is entirely possible to have both conditions simultaneously, and it is more common than many people realise. Patients with eczema have a compromised skin barrier that makes them more susceptible to developing sensitisations to contact allergens over time, meaning the two conditions can co-exist and overlap.
How do I know if my rash is contact dermatitis or eczema?
The most reliable way is to consider the location and pattern of your rash, your personal and family history, and whether a specific trigger can be identified. Contact dermatitis typically appears in areas that have come into direct contact with a substance, whereas eczema tends to follow characteristic anatomical patterns — but a clinical assessment is always the most accurate approach.
Is contact dermatitis contagious?
No — contact dermatitis is not contagious and cannot be passed from person to person. It is a reaction occurring within an individual’s own immune system in response to a substance, not an infectious condition.
Can contact dermatitis become permanent?
In most cases, contact dermatitis resolves once the trigger is identified and avoided. However, with repeated or prolonged exposure — particularly in occupational settings — the skin can become chronically sensitised, making even low-level exposures sufficient to trigger a reaction.
What is the best cream for contact dermatitis?
Treatment depends on the severity of the reaction. For mild cases, a good emollient and avoiding the trigger is often sufficient. For moderate-to-severe inflammation, a topical corticosteroid such as Eumovate or Betnovate (prescribed following a consultation) is typically recommended to reduce inflammation more effectively.
Does eczema ever go away completely?
Many children with eczema see significant improvement or complete resolution of symptoms as they reach adulthood, though this is not universal. Adult-onset eczema can be persistent, though with consistent management — regular emollient use, trigger avoidance, and appropriate treatment during flares — most patients achieve good long-term control.
Making the Right Decision for Your Skin
The path to clearer, healthier skin starts with one thing: understanding exactly what is causing your symptoms. While both conditions share a common presentation of redness, itch, and inflammation, they are driven by different mechanisms and require different management approaches. Eczema is a chronic condition that requires ongoing care and flare prevention, whereas contact dermatitis can often be significantly improved — or resolved entirely — once the trigger is identified and removed.
Whatever the cause of your skin symptoms, you do not have to manage them alone. At The Care Pharmacy, our pharmacist-led prescribing team is experienced in supporting patients with both conditions, offering clinically appropriate treatments following a confidential online consultation. Whether you are in the early stages of investigating your symptoms or looking to refine an existing treatment plan, we are here to support you.
Reach out to our team today, or complete our online consultation to explore which eczema and dermatitis treatments may be right for you.
Betnovate (betamethasone valerate 0.1%)
A potent topical corticosteroid for short-term use on moderate-to-severe eczema and contact dermatitis flares affecting the body. Available following a clinical consultation with our prescribing team.
Available following an online consultation at The Care Pharmacy.
Eumovate (clobetasone butyrate 0.05%)
A mild-to-moderate topical steroid offering effective anti-inflammatory relief with a lower risk profile — suitable for more sensitive skin areas and for use under appropriate clinical guidance.
Available following an online consultation at The Care Pharmacy.
Get the right treatment for your skin today
Begin a free, confidential online consultation with our pharmacist-led team. Treatments for eczema and contact dermatitis available, including emollients and prescription topical steroids.
This article was written by Pharmacy Mentor and clinically reviewed by Mohammed Ismail Lakhi, MPharm, MRPharm, Superintendent Pharmacist at The Care Pharmacy. Mohammed is registered with the General Pharmaceutical Council (GPhC registration number 2072815) and leads clinical governance across The Care Pharmacy’s weight management services.
Last reviewed: May 2026
Disclaimer: This article is for general information only and is not a substitute for individual medical advice. Always consult a qualified prescriber before starting any prescription weight loss treatment.
Medically reviewed by
Mohammed Lakhi
Superintendent Pharmacist










