Dermatitis on the face is one of the most distressing skin conditions to manage — not only because the symptoms are visible and difficult to conceal, but because the face is uniquely sensitive, making treatment choices more complex than for other areas of the body. Facial dermatitis is not a single condition: it is an umbrella term covering several distinct types, including contact dermatitis, seborrhoeic dermatitis, and perioral dermatitis, each with different causes, patterns, and treatment approaches. The common thread is inflammation — redness, flaking, itching, and in some cases, pustules or weeping skin that can significantly affect confidence and quality of life. Identifying which type of dermatitis you have is the essential first step, because using the wrong treatment can make symptoms considerably worse, particularly on the delicate skin of the face. Finding the right treatment for facial dermatitis does not have to be complicated. Our clinically led team is here to guide you through your options with a straightforward online consultation.
Before we explore the detail, get in touch with our team if you have questions about your skin, or complete our online consultation to find out which treatments may be right for you.
Start Your Consultation
Quick Answer
Dermatitis on the face can be caused by several distinct conditions — contact dermatitis, seborrhoeic dermatitis, and perioral dermatitis being the most common — and each requires a different treatment approach. Contact dermatitis is triggered by direct exposure to an irritant or allergen in a skincare product, cosmetic, or environmental substance. Seborrhoeic dermatitis is a chronic yeast-related condition that causes flaking and redness in oily areas of the face such as the nose, eyebrows, and hairline. Perioral dermatitis presents as a rash of small red bumps around the mouth and chin, often triggered or worsened by topical steroids. In all cases, identifying the correct diagnosis is essential before starting treatment, and a clinical consultation is the most reliable route to getting that right.
Types of Dermatitis on the Face
Every effective facial dermatitis treatment plan begins in the same place: an accurate understanding of which condition you are actually dealing with. The three most common types affecting the face each have distinct characteristics, but they can look deceptively similar — particularly during an active flare — which is why misdiagnosis and inappropriate treatment are surprisingly common.
The three main types are:
- Contact dermatitis: An inflammatory reaction triggered by direct skin contact with an irritant (irritant contact dermatitis) or an allergen (allergic contact dermatitis). On the face, common culprits include skincare products, cosmetics, fragrances, hair dye, and nickel in glasses frames or jewellery.
- Seborrhoeic dermatitis: A chronic, relapsing condition caused by an overgrowth of the yeast Malassezia on the skin surface, combined with an inflammatory response. It affects oily areas of the face — particularly the sides of the nose, eyebrows, and the hairline — and is characterised by redness, greasy scaling, and itch.
- Perioral dermatitis: A distinct inflammatory condition presenting as small red papules and pustules clustered around the mouth, chin, and sometimes the nose and eyes. It is frequently triggered or worsened by topical steroid use, heavy moisturisers, and fluorinated toothpaste.
There is also atopic dermatitis (eczema) of the face, which affects many eczema patients and tends to appear on the cheeks, around the eyes, and on the forehead, particularly in children. This shares features with contact dermatitis but is driven by a pre-existing genetic skin barrier dysfunction rather than a specific external trigger.
Getting the right diagnosis matters enormously on the face. Treatments appropriate for one type — such as a potent topical steroid for atopic eczema — can be harmful for another, such as perioral dermatitis, where steroid use is a known causative factor.
Contact Dermatitis on the Face: Causes and Symptoms
Contact dermatitis on the face is extremely common, in part because the face is the area of the body exposed to the widest range of topical products on a daily basis. Moisturisers, cleansers, serums, sunscreens, foundations, mascaras, hair dyes, and fragrances all represent potential triggers — and the more products you use, the more complex the process of identifying the culprit becomes.
Irritant contact dermatitis on the face
Irritant contact dermatitis occurs when a substance physically disrupts or damages the skin barrier without necessarily triggering an immune response. On the face, this is particularly common with:
- Over-exfoliation — excessive use of chemical exfoliants (AHAs, BHAs, retinoids) that strip the skin barrier
- Harsh cleansers with high detergent content or alkaline pH
- Repeated exposure to hand sanitiser that comes into contact with the face
- Certain active skincare ingredients used at too high a concentration or too frequently
- Face masks — both sheet masks containing sensitising ingredients and physical masks causing friction and occlusion
Allergic contact dermatitis on the face
Allergic contact dermatitis on the face involves a true immune-mediated reaction to a specific allergen. Once sensitised, even tiny amounts of the allergen can trigger a reaction. Common facial allergens include:
- Fragrances — found in almost all standard skincare, cosmetics, and hair products
- Preservatives — particularly methylisothiazolinone (MI), methylchloroisothiazolinone (MCI), and formaldehyde-releasing agents
- Hair dye chemicals — para-phenylenediamine (PPD) can cause severe reactions around the hairline, forehead, and ears
- Nickel — from glasses frames, earrings, or necklace clasps that rest against the face
- Sunscreen ingredients — particularly some chemical UV filters
- Rubber or latex — from face masks, goggles, or elastic bands
Symptoms of contact dermatitis on the face
Symptoms typically include redness, swelling, intense itch, dry or flaking skin, and in more severe cases, blistering or weeping. The distribution often follows the pattern of contact — for example, redness across both cheeks from a face cream, or a reaction along the hairline from a hair dye. Eyelid dermatitis — one of the most common and frustrating presentations — is frequently caused by contact allergens in mascara, eye cream, nail varnish (transferred by touching the eyes), or eye drops.
Seborrhoeic Dermatitis on the Face: What You Need to Know
Seborrhoeic dermatitis on the face is one of the most prevalent skin conditions in the UK, affecting an estimated 1–3% of the general population and up to 5% of adults. Despite its prevalence, it is frequently misidentified as dry skin, rosacea, or contact dermatitis — leading to months or even years of ineffective treatment.
The condition is caused by an inflammatory response to Malassezia yeast, which colonises sebaceous (oil-producing) skin. This is why seborrhoeic dermatitis characteristically affects the oiliest areas of the face:
- The sides of the nose and nasolabial folds
- The eyebrows and the skin above and between them
- The hairline and temples
- The ears and behind the ears
- The central chest and upper back (in some patients)
The characteristic appearance is of red, inflamed skin with greasy yellowish or white scaling, often accompanied by itch. Unlike contact dermatitis, the distribution is fairly predictable and symmetrical. Unlike eczema, the skin tends to be oily rather than dry in affected areas.
Key facts about seborrhoeic dermatitis on the face:
- It is a chronic, relapsing condition — it cannot be cured, but it can be managed very effectively with the right treatment
- It is not contagious and is not caused by poor hygiene
- It tends to worsen in cold, dry weather and under stress
- It is significantly more common in people who are immunocompromised, including those with HIV, and in patients with neurological conditions such as Parkinson’s disease
- Antifungal treatments — both topical and, for severe cases, oral — form the cornerstone of management
- Standard emollients and topical steroids alone are insufficient; an antifungal component is essential for meaningful improvement
If you have redness and scaling that keeps returning despite moisturising and gentle skincare, seborrhoeic dermatitis should be on your radar. Get in touch with our team if you would like clinical guidance on next steps.
Perioral Dermatitis: Causes, Symptoms, and Why It Is Often Misdiagnosed
Perioral dermatitis is a condition that causes significant distress partly because of where it appears — in the most visible, central area of the face — and partly because it is so frequently misidentified and mistreated, leading to prolonged suffering that could have been avoided with an earlier accurate diagnosis.
Perioral dermatitis causes are not fully understood, but several factors are consistently implicated:
- Topical steroid use: This is the most commonly identified trigger. Applying topical corticosteroids to the face — even mild ones — can trigger or significantly worsen perioral dermatitis. Many patients develop the condition after being prescribed a topical steroid for an unrelated facial rash, creating a cycle where stopping the steroid initially worsens symptoms, leading to further steroid use.
- Heavy moisturisers and occlusive products: Rich creams, heavy foundations, and occlusive sunscreens appear to worsen perioral dermatitis in susceptible individuals, possibly by occluding follicles and disrupting the skin microbiome.
- Fluorinated toothpaste: A notable proportion of patients report improvement after switching to a non-fluorinated toothpaste, though the evidence base for this is largely observational.
- Hormonal factors: The condition is significantly more common in women of childbearing age, and many patients notice a worsening around hormonal fluctuations.
- Inhaled corticosteroids: Use of steroid inhalers for asthma has been associated with perioral dermatitis in some patients, particularly those who do not use a spacer device.
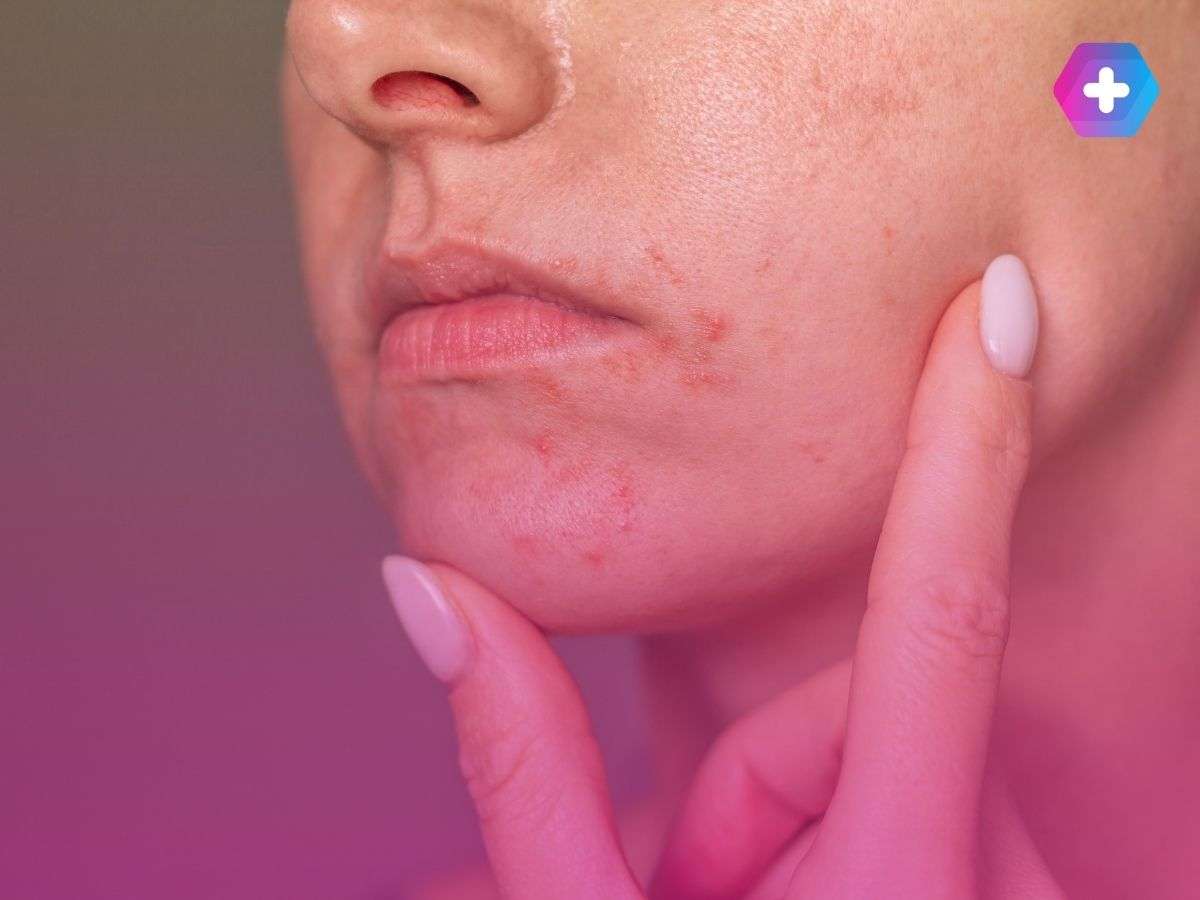
Symptoms of perioral dermatitis include clusters of small red papules and pustules — sometimes with a fine scaly texture — arranged in a ring around the mouth, typically with a clear zone of unaffected skin immediately around the lip border. The chin and nasolabial folds are also frequently involved. The rash can extend to the nose (perinasal) or around the eyes (periocular dermatitis).
The most important and counterintuitive aspect of perioral dermatitis treatment is this: topical steroids must be stopped, even though stopping them initially causes a rebound flare. This steroid withdrawal phase — during which symptoms temporarily worsen before improving — is one of the main reasons patients abandon treatment prematurely. Clinical support during this phase is invaluable. Complete our online consultation to discuss your symptoms with our prescribing team.
Facial Dermatitis at a Glance: A Comparison
The table below summarises the key differences between the three main types of facial dermatitis to help you identify which condition may be affecting your skin:
Feature
Contact Dermatitis
Seborrhoeic Dermatitis
Perioral Dermatitis
Primary cause
Irritant or allergen contact
Malassezia yeast overgrowth
Topical steroids, heavy products, hormones
Location on face
Follows pattern of contact — cheeks, eyelids, hairline
Nose, eyebrows, hairline, ears
Around the mouth, chin, nose, and eyes
Appearance
Red, inflamed, possibly blistering or weeping
Red with greasy yellowish or white scaling
Small red papules and pustules in clusters
Skin texture
Dry, flaky, or weeping
Oily with greasy scale
Fine scale or smooth papules
Chronic or acute?
Resolves when trigger removed
Chronic and relapsing
Persistent until correctly treated
Role of topical steroids
May help reduce inflammation short-term
Limited role; antifungals are primary treatment
Contraindicated — steroids worsen the condition
First-line treatment
Trigger removal; emollient; mild topical steroid if needed
Topical antifungal; medicated shampoo or wash
Stop topical steroids; topical or oral antibiotic
Who is most affected?
Anyone; more common in those using multiple skincare products
Adults; more common in men and immunocompromised patients
Women of childbearing age predominantly
Facial Dermatitis Treatment: What Works and What to Avoid
Facial dermatitis treatment requires a more careful approach than treating dermatitis elsewhere on the body. The skin on the face — particularly around the eyes, on the eyelids, and in nasolabial folds — is significantly thinner and more permeable than body skin, meaning that topical treatments are absorbed more readily and carry a higher risk of side effects if used incorrectly.
General principles for treating facial dermatitis:
- Identify and remove the trigger before reaching for a treatment — particularly for contact dermatitis, where continuing exposure will prevent recovery regardless of what product you apply
- Simplify your skincare routine radically during a flare. A gentle, fragrance-free cleanser and a basic unfragranced emollient is the safest starting point
- Avoid all potentially sensitising products — including retinoids, chemical exfoliants, vitamin C serums, and fragranced products — until the skin has fully recovered
- Never apply a topical steroid to the face without clinical guidance, and never use a potent steroid on facial skin
- Be patient — facial dermatitis takes longer to resolve than body dermatitis in many cases, and rushing treatment often worsens outcomes
Treatment by type:
For contact dermatitis on the face, removing the trigger is the primary intervention. A mild topical corticosteroid such as Eumovate (clobetasone butyrate 0.05%) may be used under clinical guidance for short periods to reduce inflammation. Eumovate is a mild-to-moderate steroid with a well-established safety profile for facial use when used correctly and for brief treatment courses only. Potent topical corticosteroids such as Betnovate are not suitable for use on facial skin and should only be used on body areas under clinical supervision.
For seborrhoeic dermatitis on the face, antifungal treatments are the cornerstone of management. Topical ketoconazole cream is the most widely used first-line option, applied to affected areas once or twice daily. Maintenance treatment — applying antifungal products less frequently once remission is achieved — is important for preventing relapse, as the condition is chronic.
For perioral dermatitis, treatment involves stopping all topical steroids (with clinical support to manage the rebound phase), eliminating heavy products, and introducing a topical or oral antibiotic. Topical metronidazole and oral tetracyclines such as doxycycline or lymecycline are the most commonly prescribed options. Recovery can take two to three months with consistent treatment.
What to avoid on facial dermatitis:
- Potent topical steroids — the risk of skin thinning, telangiectasia, and steroid-induced rosacea on the face is significant with prolonged use
- Fragranced moisturisers, toners, or serums — fragrance is one of the most common contact allergens on the face
- Physical or chemical exfoliants during active flares — these further damage an already-compromised barrier
- Multiple new products introduced simultaneously — this makes it impossible to identify the cause of any reaction
- Self-prescribing topical steroids from previous prescriptions — strength, duration, and appropriateness must be clinically assessed for facial use each time
Gentle Products That Support Facial Dermatitis
When your face is inflamed, reactive, and uncomfortable, reaching for the right products can make a significant difference — both in terms of settling symptoms and in protecting the skin barrier from further damage. The following products are appropriate for facial dermatitis and are available through our pharmacy following consultation where clinically required.
Eumovate Cream (clobetasone butyrate 0.05%)
Eumovate Cream is a mild-to-moderate topical corticosteroid with a well-established clinical record of safe use on facial skin when applied correctly. It is appropriate for short-term treatment of contact dermatitis and atopic eczema flares on the face under clinical guidance, offering meaningful anti-inflammatory relief without the higher risk profile of potent steroids.
It is important to note that Eumovate is not appropriate for seborrhoeic dermatitis (where antifungal treatment is required) and is contraindicated for perioral dermatitis. Clinical guidance before use on the face is strongly recommended.
Betnovate Cream (betamethasone valerate 0.1%)
Betnovate Cream is not suitable for use on facial skin and should only be used on body areas under clinical supervision. It is included here for completeness as part of our eczema and dermatitis range, and is appropriate for moderate-to-severe eczema flares affecting the body when prescribed following a clinical assessment. Never use on the face, eyelids, or periorbital skin. Prescription only.
All products are available following a clinical consultation with our prescribing team. Complete our online consultation to find out which option is right for your skin.
Practical Steps for Managing Dermatitis on the Face
Managing facial dermatitis requires consistency, patience, and a willingness to make sometimes significant changes to your skincare routine. The following ten tips are grounded in clinical evidence and designed to make a real difference to your skin:
- Strip your routine back to the absolute minimum. During an active flare, use only a fragrance-free soap substitute and a basic unfragranced emollient. Introduce additional products one at a time, waiting two to four weeks between each introduction, once your skin has fully settled.
- Switch to a fragrance-free soap substitute for cleansing. Standard facial cleansers — even those marketed as gentle or sensitive — frequently contain surfactants and fragrances that worsen facial dermatitis. Epaderm Cream used as a soap substitute is a clinically appropriate and effective alternative.
- Photograph your skin regularly. Progress with facial dermatitis can be difficult to see on a day-to-day basis. Weekly photographs taken in the same light give you an objective record of whether your skin is improving, stable, or worsening — which is valuable information for both you and your prescriber.
- Check every product for fragrance and common preservatives. Look for methylisothiazolinone (MI), methylchloroisothiazolinone (MCI), formaldehyde-releasing preservatives, and any ingredient listed as “parfum” or “fragrance.” These are among the most common facial contact allergens.
- Do not use topical steroids on the face without specific clinical guidance. Even mild topical steroids should be used on facial skin for short, defined courses only, and potent steroids should never be used on the face routinely. Always seek clinical advice before applying any steroid product to facial skin.
- Be cautious with SPF products during a flare. Sunscreen is important for protecting inflamed skin, but many standard sunscreens contain fragrances, chemical UV filters, or preservatives that can worsen facial dermatitis. Look for mineral sunscreens containing only zinc oxide or titanium dioxide, which are generally better tolerated on reactive skin.
- Check your hair products as well as your skincare. Shampoos, conditioners, hair dyes, and styling products run down onto the face, neck, and ears during use — and are a surprisingly common cause of facial contact dermatitis, particularly around the hairline and on the eyelids.
- Change your pillowcase every two to three days. Pillowcases accumulate skincare product residue, sweat, and skin cells that can re-expose your face to potential irritants and allergens every night. Switching to a fresh pillowcase frequently is a simple but effective habit during a flare.
- Manage internal triggers alongside topical treatment. Stress, sleep deprivation, and illness can all worsen facial dermatitis — particularly atopic and seborrhoeic types. Addressing these factors as part of your overall management plan produces better outcomes than topical treatment alone.
- Seek a clinical review promptly if symptoms are not improving. Facial dermatitis that does not respond to basic trigger avoidance and barrier repair within two to four weeks warrants clinical assessment. Prolonged untreated facial inflammation can lead to post-inflammatory hyperpigmentation and skin barrier changes that take considerably longer to resolve. Our team is here to help — get in touch at any point.

Frequently Asked Questions
Here are the questions patients most commonly ask our prescribing team about dermatitis on the face:
How do I know if I have seborrhoeic dermatitis or rosacea on my face?
Both conditions cause facial redness and can look similar, but there are key differences. Seborrhoeic dermatitis typically produces greasy scaling in oily areas such as the nose and eyebrows, while rosacea tends to cause persistent central facial flushing, visible blood vessels, and in some cases papules and pustules without the greasy scale. A clinical assessment is the most reliable way to differentiate between the two, as treatment approaches differ significantly.
Can I use hydrocortisone cream on my face for dermatitis?
Over-the-counter hydrocortisone 1% is not recommended for use on the face without medical advice, and should never be used around the eyes or on the eyelids. A clinical consultation is recommended before applying any corticosteroid to facial skin, as appropriate strength, duration, and suitability must be individually assessed.
Why does my facial dermatitis keep coming back?
Recurring facial dermatitis is usually a sign that an underlying trigger has not been fully identified and removed, or that a chronic condition such as seborrhoeic dermatitis is not being managed with an appropriate maintenance routine. A detailed skin history and, where relevant, patch testing to identify contact allergens is often the most effective way to break the cycle of recurrence.
Can makeup cause dermatitis on the face?
Yes — makeup is one of the most common sources of contact allergens on the face, with fragrances, preservatives, dyes, and certain pigments all capable of triggering allergic or irritant contact dermatitis. If you suspect makeup is contributing to your facial dermatitis, removing all cosmetics from your routine for two to four weeks and monitoring your skin is a practical first step, before reintroducing products individually to identify the culprit.
Is perioral dermatitis the same as acne?
No — although perioral dermatitis can superficially resemble acne due to the presence of small papules and pustules, the two conditions are distinct and require different treatments. Perioral dermatitis is not caused by blocked pores or excess sebum, does not respond to standard acne treatments such as benzoyl peroxide or salicylic acid, and is specifically associated with topical steroid use — which, unlike acne, is a contraindicated treatment for perioral dermatitis.
How long does facial dermatitis take to clear?
This depends heavily on the type and severity of the condition and whether the trigger has been identified and removed. Contact dermatitis typically begins to improve within one to two weeks once the trigger is removed and appropriate treatment is in place, though complete resolution may take four to six weeks. Perioral dermatitis can take two to three months to resolve fully, and seborrhoeic dermatitis, being a chronic condition, requires ongoing maintenance rather than a defined treatment course.
Calmer, Clearer Skin Is Within Reach
Treating your skin effectively is not about using the strongest product available. It is about using the right one for your specific skin and condition — and on the face, where the stakes are higher and the margin for error is smaller, getting that right matters more than anywhere else. Whether you are dealing with contact dermatitis triggered by a product in your routine, the persistent flaking of seborrhoeic dermatitis, or the frustrating clusters of perioral dermatitis, the right clinical approach can transform your skin and your confidence.
At The Care Pharmacy, our pharmacist-led prescribing team is here to help you navigate your options, identify the right diagnosis, and access the treatments that will make a genuine difference. Getting the right treatment should not require a lengthy wait or an in-person appointment — our confidential online consultation is designed to make that process as straightforward as possible.
Reach out to our team today, or complete our online consultation to explore which eczema and dermatitis treatments are right for your skin.
Eumovate Cream (clobetasone butyrate 0.05%)
A mild-to-moderate topical corticosteroid with a well-established record of safe facial use for contact dermatitis and eczema flares when used as directed. Short-term use only. Not suitable for seborrhoeic or perioral dermatitis.
Available following an online consultation at The Care Pharmacy.
Betnovate Cream (betamethasone valerate 0.1%)
Not suitable for use on facial skin. Betnovate is included as part of our eczema and dermatitis range for body use only, under clinical supervision. Appropriate for moderate-to-severe eczema flares on the body following a clinical consultation. Never use on the face, eyelids, or periorbital skin. Prescription only.
Available following an online consultation at The Care Pharmacy.
Find the right treatment for your skin today
Begin a free, confidential online consultation with our pharmacist-led team. Prescription and non-prescription treatments for facial dermatitis available following assessment.
This article was written by Pharmacy Mentor and clinically reviewed by Mohammed Ismail Lakhi, MPharm, MRPharm, Superintendent Pharmacist at The Care Pharmacy. Mohammed is registered with the General Pharmaceutical Council (GPhC registration number 2072815) and leads clinical governance across The Care Pharmacy’s weight management services.
Last reviewed: May 2026
Disclaimer: This article is for general information only and is not a substitute for individual medical advice. Always consult a qualified prescriber before starting any prescription weight loss treatment.
Medically reviewed by
Mohammed Lakhi
Superintendent Pharmacist










